The End of the COVID-19 Public Health Emergency: New Deadlines for Group Health Plans
Employee Benefits Alert
With the COVID-19 Public Health Emergency (PHE) set to end on May 11, 2023, federal agencies have published FAQs explaining how the end of the PHE will affect previously extended deadlines relating to COBRA, HIPAA special enrollment, and claims and appeals under group health plans. This article provides (i) a recap of the deadlines, (ii) rules of thumb for determining the deadlines, and (iii) tables more specifically addressing some of the most common deadlines that arise. Plan administrators should review plan operations now and prepare to administer these shifting deadlines correctly to avert potential penalties and minimize avoidable claims exposure.
Deadlines Subject to Extensions
In prior articles, we described the original actions taken by federal agencies to extend these deadlines and further guidance describing how the extensions are calculated. Specifically, the following deadlines have been extended through the earlier of one year from the applicable date or 60 days after the end of the PHE, which is expected to be July 10, 2023:
- 30-day period (or 60-day period, if applicable) to request special enrollment under HIPAA;
- Date for providing a COBRA election notice;
- 60-day election period for COBRA continuation coverage;
- Date for making COBRA premium payments;
- Date for individuals to notify the plan of a qualifying event or determination of disability with respect to COBRA;
- Date by which individuals may file a benefit claim under the plan’s claims procedure;
- Date by which claimants may file an appeal of an adverse benefit determination under the plan’s claims procedure;
- Date by which claimants may file a request for an external review after receipt of an adverse benefit determination or final internal adverse benefit determination; and
- Date by which a claimant may file information to perfect a request for external review upon a finding that the request was not complete.
Rules of Thumb for Determining Deadlines
The following rules of thumb can be helpful for applying the extensions of the deadlines described above:
- If the countdown to the deadline would have started before July 11, 2022, the countdown begins after one year has passed.
- If the countdown to the deadline would have started from July 11, 2022, through July 10, 2023, the countdown begins on July 11, 2023.
- If the countdown to the deadline starts to run on or after July 11, 2023, the countdown begins as usual.
Tables Illustrating Common Deadlines
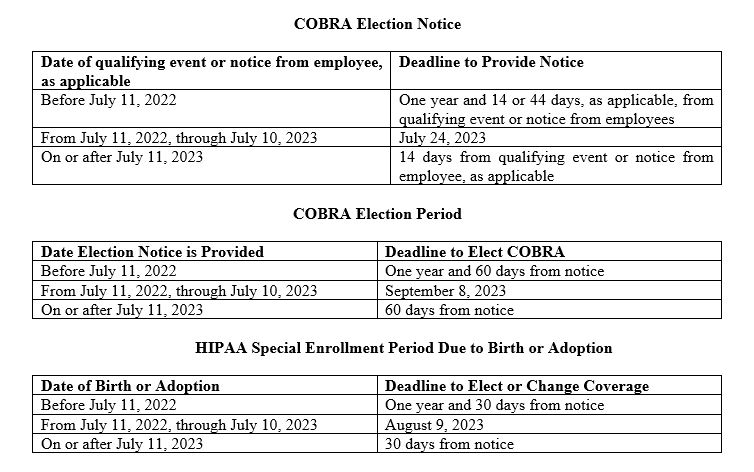
The following tables illustrate the above rules of thumb as applied to three of the most common deadlines that are likely to arise: (1) the deadline to furnish a COBRA election notice, (2) the deadline to elect COBRA continuation coverage, and (3) the deadline to elect HIPAA special enrollment due to a birth or adoption.
If you have any questions about how the end of the PHE might affect your plan, please contact one of the attorneys in the Employee Benefits and Executive Compensation Practice Group at Bradley.

